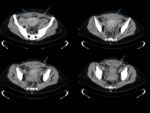
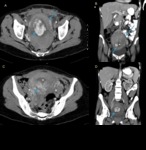
Protocol
Most of the studies included in this review were performed with a MDCT-40 Siemens Somathon scanner.
Abdominopelvic CT scans from the diaphragm to the symphysis pubis were obtained with a 20 x1.5 mm detector configuration,
a reconstruction interval of 4/1.5 mm,
and a tube rotation time of 0.35 s.
Nonionic intravenous contrast material (dose of 2 mL/Kg at a rate of 3 ml/s) was routinely administered.
A scan delay of 70 seconds after the beginning of intravenous contrast material injection was employed,
thus,
obtaining a portal venous phase.
Delayed excretory phase was obtained when confusing images were found in the portal venous phase for bladder and ureteral opacification.
Oral contrast (750-1000 ml of a 3% iodinated solution,
Gastrografin) was administered in some cases.
Multiplanar reconstruction (MPR) and volume rendering imaging were also realized in some cases.
Imaging findings:
MDCT findings that allows obviating the immediate ultrasonography
There are 4 situations in which CT evaluation of pelvis of a woman allows obviate the immediate ultrasonography:
1.
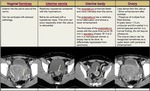
Gynecologic structures have normal CT appearance.
If a CT examination shows the absence of ovarian,
tubal,
or uterine morphological alteration re-evaluation of the pelvis with US in the acute setting may no longer be necessary.
The radiologist should be cognizant of the spectrum of normal appearance of these structures in both pre and postmenopausal women to avoid misinterpreting them as abnormal.
The normal CT appearance of the gynecologic structures is described in table 1.
2.
The anomaly has a limited differential diagnosis and follow-up is required.
Under this headland we include several cystic adnexal lesions that are listed along with their characteristic appearance on CT in table 2.
CT identification of a smooth walled ovarian cyst with fluid attenuation should almost never require reimaging with US.
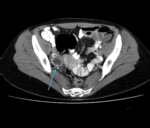
The differential diagnosis for the CT finding is nonneoplastic cyst,
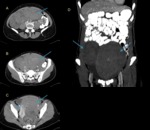
the most common being follicular cysts (fig 1),
versus benign neoplasm.
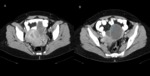
Approximately 50–70% of serous epithelial ovarian tumors are benign,
with a peak in these benign serous cystadenomas in the fourth and fifth decades.
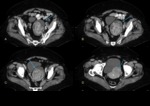
Serous cystadenomas are typically unilocular,
thin-walled cystic masses,
with an average size of 10 cm in diameter,
and may be bilateral in 12–20% of cases (Fig.
2).
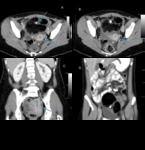
Mucinous cystadenomas are less common than serous tumors and peak in the third to fifth decades.
These tumors may be even larger than serous cystadenomas and are typically multilocular cystic masses with very thin septations.
Ultrasound would be appropriate as the subsequent follow-up examination when deemed necessary,
but it would be most useful 3 to 6 months later.
Even when the cyst has internal density higher than simple fluid,
immediate reimaging with US would be of no benefit in the premenopausal woman if a well defined cyst wall is clearly depicted on CT.
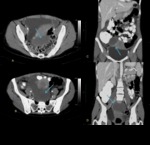
The differential diagnosis for such a lesion would be acute hemorrhagic cyst (high prevalence) versus endometrioma (medium-low prevalence,
affecting about 10% of premenopausal women,
fig 3) versus benign neoplasm containing hemorrhage or high-density mucin (relatively rare).
Follow-up observation would be required to distinguish between these possibilities.
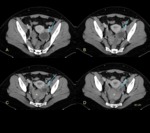
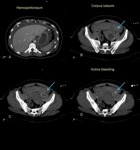
One of the most common gynecologic causes of acute pelvic pain in a premenopausal woman is hemorrhage into a follicular or corpus luteal cyst.
Subsequent rupture of this hemorrhagic cyst may,
then,
result in hemoperitoneum (fig 4),
often with associated abdominal as well as pelvic pain and hypotension.
In women of reproductive age,
the gynecologic tract is the most common source of spontaneous hemoperitoneum,
with rupture of ovarian cysts and ectopic pregnancy as the primary etiologies.
The detection of significant hemoperitoneum on CT should prompt surgical consultation without delay.
MDCT images can demonstrate active extravasation,
which manifests as pooling of contrast-enhanced blood in the pelvis.
3.
CT finding has characteristic diagnostic appearance.
There are a number of gynecologic conditions that have a characteristic appearance on CT that precludes the necessity for further imaging evaluation and are described in table 3.
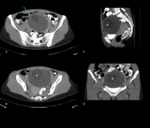
Teratomas represent 96% of germ-cell tumors and 15% of all ovarian tumors.
The vast majority of teratomas are mature and benign,
with 99% demonstrating a cystic component.
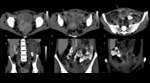
On CT images,
regions with fat attenuation are observed in more than 90% of cases.
On CT,
the presence of calcium or fat within a pelvic mass is diagnostic (fig 5).
They are bilateral in 15%–20% of cases and are associated with torsion in more than 15% of cases (fig 14).
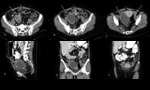
When adhesions obstruct the fimbriated end of the fallopian tube,
hydrosalpinx results because of the accumulation of intraluminal secretions.
A tubular structure,
especially when it exhibits a waist sign or is clearly separate from the ipsilateral ovary,
is a hydrosalpinx (fig 6).
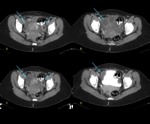
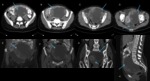
Pelvic inflammatory disease (PID) is one of the most common causes of acute pelvic pain in sexually active women.
PID should be suspected in all patients presenting with pelvic pain/cervical motion tenderness,
fever,
and leukocytosis.
Neisseria gonorrhoeae or Chlamydia trachomatis is believed to be the offending agent in two-thirds of cases,
but polymicrobial infection also has been reported.
Infection usually ascends from a cervicitis to involve the uterus,
and then progresses to salpingitis.
If treatment is delayed,
the infection can ultimately result in pyosalpinx,
tuboovarian complex,
and abscess potentially necessitating radiologic or surgical drainage.
The imaging findings vary depending on disease severity (Fig 7-9).
Although clinical history,
laboratory findings and US are usually sufficient to reach a diagnosis of PID,
CT can often provide additional information,
including the presence of ureteral obstruction due to adnexal inflammation,
the spread of inflammation to the perihepatic space (Fitz-Hugh and Curtis syndrome),
or the presence of nongynecologic sources of pelvic pain.
If the diagnosis is adequately established by virtue of the CT findings in combination with the clinical history,
further evaluation with US is of doubtful additional benefit.
In premenopausal women with indeterminate ovarian masses,
there is approximately an 8.75% risk of malignancy.
This risk rises in a postmenopausal woman,
to approximately 32.4%.
Differentiation of benign cystic masses such as serous or mucinous cystadenomas from malignant versions of the same tumors is critical in determining the appropriate surgery for these patients.
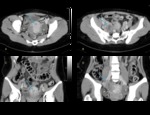
Ovarian cancer often presents as a large solid and cystic adnexal mass,
with obvious CT features (fig 10).
Enlarged parauterirne,
ovarian and pelvic veins may be observed on CT in patients who have no corresponding symptoms (fig 11). Clinical history is important to distinguish between symptomatic pelvic varices and incidental pelvic varices.
4.
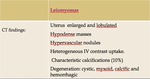
CT shows abnormality to be myometrial in origin.
Leiomyomas (fig 12 and 13) are common benign tumors of the uterus (more than 20 % of women over the age of 30 years) composed of smooth muscle cells interspersed with fibrous connective tissue.
Fibroids are predominantly found in women of reproductive age and may enlarge during pregnancy or during oral contraceptive use,
with a tendency to regress in the postmenopausal state.
Although fibroids may be asymptomatic,
women may present with acute pelvic pain in the case of degeneration or infarction,
or in the rare event of torsion of an exophytic fibroid. The main CT findings are summarized in table 4.
When to consider US after MDCT
1.-To identify the ovary and its relationship to the observed anomaly if it has not been possible with CT.
2.-To clarify the vascularity of the observed anomaly especially in non contrast CT if ovarian torsion is suspected.
Torsion of the ovary or,
more frequently,
the adnexa (ovary and fallopian tube) accounts for approximately 3% of emergency gynecologic surgeries.
Torsion can occur at any age,
however,
is rare in the postmenopausal patient.
In adults,
it is often associated with an ovarian cyst or benign neoplasm.
CT findings of ovarian torsion are somewhat nonspecific and are described in table 5.
If findings indicative of torsion are found on CT in a patient in whom the gynecologist strongly suspects torsion,
the patient will reasonably go directly to surgery without a confirmatory US.
CT-detected unilateral ovarian enlargement is not by itself diagnostic of ovarian torsion; if there were no other CT findings that sufficiently indicate ovarian torsion (fig 14),
reimaging with US would be of value in assessing ovarian vascularity and appearance.
Clinical situations in which US is the diagnostic procedure of Choice
Possible endometrial pathology and pregnancy are clinical indications for which US is uniquely qualified to evaluate.
If endometrial thickening is discovered on a CT scan performed for pelvic pain in a premenopausal woman,
sonographic reimaging within a week of the last day of menstruation is probably the best means for determining if the endometrium is truly abnormal.
In a postmenopausal woman,
if endometrial thickening is suspected,
sonographic reimaging should be initiated,
with endometrial sampling performed if the suspected thickening is confirmed sonographically.
Because endometrial cancer is not a disease requiring emergency care,
the reimaging effort can proceed outside the emergency setting.
Although most female patients of child-bearing age should be appropriately tested for possible pregnancy before CT,
an emergent study might occur before such testing.
With an incidence of approximately 1 out of every 200 diagnosed pregnancies,
ectopic pregnancy remains the leading cause of maternal death in the first trimester and the second leading cause of maternal mortality overall. Although ultrasound is the imaging modality of choice for the diagnosis of ectopic pregnancy we must recognize the signs of this complication when CT is performed without suspecting this diagnosis (fig 15).
Situations in which MDCT is of Choice
In postpartum conditions,
CT is typically the imaging modality of choice for evaluation.
Endometritis is particularly common in women who undergo cesarean section 6 or more hours after rupture of membranes.
Another postpartum complication that may result in fever and abdominal pain is ovarian vein thrombosis,
which is right-sided in 80–90% of cases.
The main CT findings of these 2 complications are summarized in table 6.
Other possible postpartum complications include abscesses,
necrotizing fasciitis,
and colovaginal fistula.
Cesarean section may also result in infectious complication of surgical incision (see fig 16).
Uterine atony and retained products of conception (RPOC) are the most common causes of postpartum hemorrhage.
Uterine atony is seen in the immediate postpartum period,
whereas RPOC is seen later.
RPOC is suggested sonographically when an echogenic mass is present in the endometrial cavity which can contain hiperechogenic foci due to usual placenta calcification after 33 week’s gestation.
When RPOC present late after delivery,
calcifications may be secondary to the chronicity of the process.
An intrauterine clot may be confused with RPOC.
On CT,
RPOC also can appear as a high-density mass in the endometrial cavity.
If blood flow is visualized into the mass there is additional evidence that the mass represents vascularized placental tissue rather than hematoma.
After contrast administration,
enhancement of the eccentric mass supports the diagnosis (fig 17).